
If you've ever used opioids, you might already know what withdrawal feels like, or maybe you’ve supported someone you love through the experience. Nausea, anxiety, cravings, sleepless nights, and physical pain make withdrawal something that many people understandably fear.
For people considering medications for opioid use disorder like buprenorphine or naltrexone, the possibility of experiencing what’s known as “precipitated withdrawal” can be a roadblock on the path to recovery.
Precipitated withdrawal is a sudden, intense withdrawal that can happen when a person first starts taking OUD medications after stopping opioids. Luckily, precipitated withdrawal is short-lived, but it’s essential to work with your provider to start medication at the right time and at the right dose. This will reduce the risk and ensure that treatment is safe and successful.
Precipitated withdrawal can be caused by Suboxone and other medications that contain buprenorphine, naltrexone, and naloxone. While unpleasant, these symptoms are temporary. They don’t last as long as they might in typical withdrawal, and you can usually prevent them with the right timing and support.
This article will explain what precipitated withdrawal is, why it happens, and how it feels. We’ll also look at how providers at Boulder Care can help you prevent it and cope with symptoms if you do experience this type of withdrawal.
Precipitated withdrawal is a sudden, intense onset of opioid withdrawal symptoms that can occur when starting medications to stop opioid use. It happens most often with medication-assisted treatment (MAT), when buprenorphine or naltrexone is taken before opioids have fully cleared from the body. The medication rapidly displaces opioids from brain receptors, triggering sudden withdrawal.
In MAT, timing plays a big role in whether precipitated withdrawal happens. "The biggest protective step is timing," says Patricia Pechter, MD, DABFM, a clinical quality improvement physician at Boulder Care.
After stopping opioids, it’s important to wait until withdrawal symptoms begin. "Buprenorphine works best when opioids have already started to leave the body,” Dr. Pechter says. “Starting too soon can push other opioids off receptors suddenly, which is what triggers precipitated withdrawal."
Precipitated withdrawal happens when a medication–including buprenorphine–is taken too soon in medication-assisted treatment. In these situations, the medication doesn't ease withdrawal. It instead pushes the opioids that are still in the body off the receptors, triggering a sudden and often intense withdrawal.
"Buprenorphine has a very high affinity (stickiness) at the mu-opioid receptor but is only a partial agonist (activator) of this receptor," explains Ilana Hull, MD, a collaborating physician at Boulder Care.
"If buprenorphine is started after chronic use of a full agonist like heroin, fentanyl, methadone, or oxycodone, the buprenorphine can abruptly kick the full agonist off the receptor, which can lead to precipitated withdrawal," Dr. Hull says.
Precipitated withdrawal happens fast, which is often why it feels so distressing. Symptoms can appear within minutes to an hour, and that speed can make them feel more overwhelming than "regular" withdrawal might. That can be frustrating when you're expecting your medication to give you relief and instead get the opposite.
But that isn't a sign that MAT isn't working or that you've done something wrong. It’s typically a matter of timing and can happen in situations where:

Not all MAT medications have this effect. Instead, it's specifically linked to drugs that partially activate opioid receptors or block them entirely, including:
Precipitated withdrawal can feel overwhelming, due to its speed and intensity. Unlike regular withdrawal, where the symptoms build gradually, precipitated withdrawal can feel like you are being ‘thrown’ into withdrawal all at once.
People often report feeling a sudden, intense physical discomfort and rapid worsening of symptoms. That can catch people off guard, since they were expecting medication to relieve symptoms, not trigger them.
Danielle Bellosi, a peer supervisor and certified recovery coach at Boulder Care, shares her experience: "For me, precipitated withdrawal felt like withdrawal that started instantly instead of gradually. I felt hot and cold at the same time and was sweating constantly. I couldn’t get comfortable no matter how I positioned myself."
Bellosi continues, "My skin felt like it was crawling, I had post-nasal drip, and my stomach was very upset. I was exhausted but unable to actually sleep."
People may experience a range of symptoms from mild to severe.
Uncomfortable symptoms
Severe symptoms
Sometimes, the combination of physical discomfort, anxiety, and rapid onset can make the symptoms feel overwhelming without medical support.

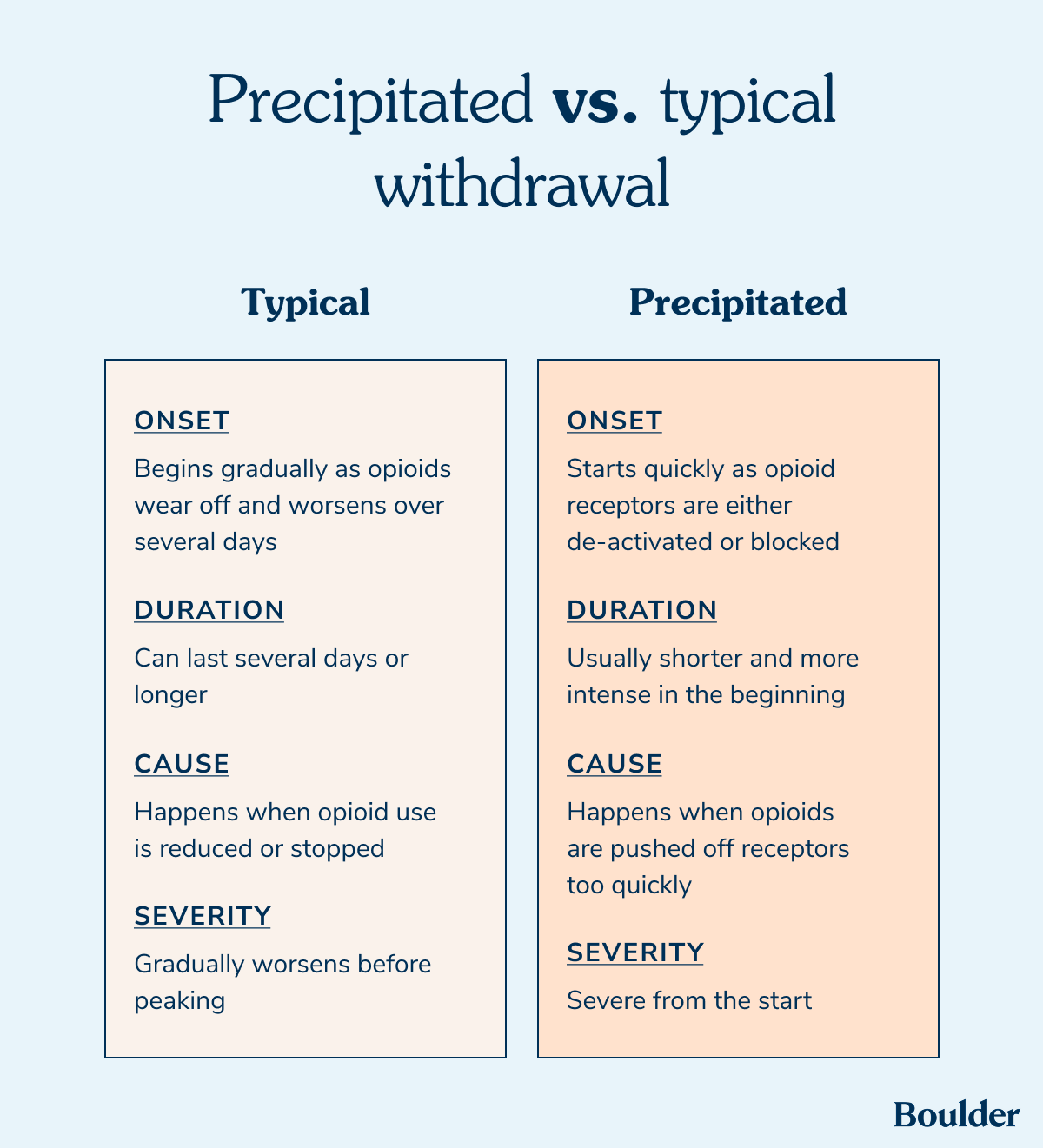
Precipitated withdrawal and typical opioid withdrawal can feel a lot alike, but differ in how quickly they start, how intense they feel, and what causes them.
While precipitated withdrawal doesn’t last as long, its sudden and intense symptoms make it feel harder to manage.
For most people, symptoms of precipitated withdrawal last about 6 to 24 hours. After peaking, some mild symptoms may continue for a day or two as the body adjusts.
“For me, the most intense part was at the beginning. The peak symptoms lasted a few hours—it felt overwhelming in the moment, but it wasn’t endless. After that initial period, I started to notice gradual relief over the rest of the day,” Bellosi says.
The good news is that symptoms are short-lived. Once the medications have stabilized opioid receptors, symptoms will begin to improve.
Factors that can affect how long precipitated withdrawal lasts include:
While precipitated withdrawal can be uncomfortable, it isn’t a medical emergency in most cases. That means that you can manage the symptoms on your own with self-care as you wait for your body to adjust to your medication.
"Treatment focuses on comfort while the body stabilizes on buprenorphine," Dr. Pechter says. This may involve:
"Having a clear explanation behind the symptoms made it easier to tolerate because I understood my body was reacting to the medication transition, not that something had gone wrong," Bellosi says.
Experiencing precipitated withdrawal doesn't mean that treatment isn't working. It can be a common part of treatment, and people who go through it are able to stabilize and continue on their MAT medication successfully.
With support from Boulder Care and the right adjustments, your treatment can be safe, effective, and life-changing.
Yes, with careful planning, precipitated withdrawal is often preventable.
The best way to minimize your risk is to work closely with your provider ahead of time to make a transition plan. They can guide you through the timing and dosing as you begin taking buprenorphine to reduce the likelihood of developing precipitated withdrawal.
This is done by waiting to start treatment when your body is ready. Timing is critical. Starting buprenorphine too early is the most common reason why precipitated withdrawal happens.
That said, precipitated withdrawal can still happen even when everything is done correctly. For example, while precipitated withdrawal with Suboxone is uncommon, it's more likely if opioids like fentanyl are still active in your system. One study found that almost 37% of people who had taken fentanyl within the previous 24 hours experienced severe withdrawal after taking buprenorphine.
It's important to tell your provider:
Having this information can help your provider choose the best dose and timing for you. Taking Suboxone or another medication containing buprenophine too soon after you last took opioids makes the risk of precipitated withdrawal much higher.
Starting buprenorphine when there are opioids still active in your body makes it more likely you'll experience precipitated withdrawal. That's why providers use tools like the Clinical Opiate Withdrawal Scale (COWS) and Subjective Opiate Withdrawal Scale (SOWS) to help determine when it's safe to begin medication.
"Waiting until you’re in 'moderate withdrawal’ lowers that risk. Moderate withdrawal generally sets in 1-3 days after taking opioids," Dr. Pechter explains. She says that at that point, people typically experience three or more of the following symptoms:
"Dose strategy matters, too," Dr. Pechter says. "There isn’t one single way to transition. Some people use standard starts, others use slower 'micro-dosing' approaches that ease the body onto buprenorphine more gradually.
That’s why your provider might recommend a different induction timeline to help reduce your risk of precipitated withdrawal. They might suggest:
“Talking with your clinician about your recovery goals, timeline, and prior withdrawal experiences helps shape a plan that fits your life rather than forcing you into a rigid schedule," Dr. Pechter explains.
While precipitated withdrawal can happen, most people who start MAT do not experience severe symptoms. Knowing what to expect and preparing for it can be helpful.
“It also helps to prepare before the transition begins,” Dr. Pechter says. “Your clinician will often prescribe medications to manage specific symptoms like anxiety, nausea, diarrhea, and sleep disruption. Having those medications ready ahead of time can make the difference between feeling overwhelmed and feeling supported.”
According to Dr. Pechter, this commonly includes medications to treat:
Just remember, as scary as precipitated withdrawal may feel in the moment, it is temporary. It also doesn't happen to everyone. And Boulder Care is here to help you through your recovery experience so that you feel safe, supported, and ready to move forward with confidence.
If you are considering taking buprenorphine, are worried about precipitated withdrawal, or have experienced it in the past, call 888-422-6530 to get guidance and support personalized for your needs.
Precipitated withdrawal can be uncomfortable and distressing, but it is not usually life-threatening. Symptoms can feel very strong, and their suddenness can be scary when you aren't anticipating it or don't know why it's happening. That's why it's so important to contact your provider if it happens. They can provide medical guidance and safely manage your symptoms so you can continue your recovery journey. “If symptoms do not improve, it is important to seek emergency medical care,” says Dr. Hull.
Yes. Precipitated withdrawal is temporary and usually short-lived. Symptoms often peak within a few hours and then improve over the next day or two. This can be very uncomfortable, but it generally starts to get better as the body adjusts to buprenorphine. Even though it will go away, it's still important to stay in touch with your provider. They can help you deal with symptoms, make adjustments, and prescribe comfort medications to help you feel better.
You may need to take more Suboxone than you started with, but do not take more than prescribed without talking to your provider first. If you're wondering how to stop precipitated withdrawal, the safest approach is to contact your provider right away. In some cases, they may recommend taking more buprenorphine to manage symptoms.
No, you should not stop treatment if you experience precipitated withdrawal. While frustrating, remember that it's a temporary reaction that can happen when buprenorphine is first introduced. Stopping your medication can actually increase the risks of further withdrawal symptoms and a return to opioid use. Instead, talk to your provider so they can adjust your treatment plan.
Precipitated withdrawal is generally an uncommon experience. Research conducted by the National Institutes of Health found that less than 1% of people with opioid use disorder experience precipitated withdrawal when starting buprenorphine. This includes people taking long-acting opioids like fentanyl. Another study of ER patients placed the number at around 12%.
At Boulder Care, we’re committed to providing clear, evidence-based information about opioid and alcohol use disorder recovery. Learn more about our editorial standards and medical review process.