
Treatment decisions for opioid addiction can sometimes be complex, particularly when there are multiple options that seem similar. Growing up with a parent who struggled with substance use, I remember how confusing the treatment process felt—not just for them, but for the entire family. Treatment options were often poorly explained, leaving them unsure of whether they were making the right choice.
For people considering medication-assisted treatment for opioid use disorder, buprenorphine is often a big part of those treatment conversations.
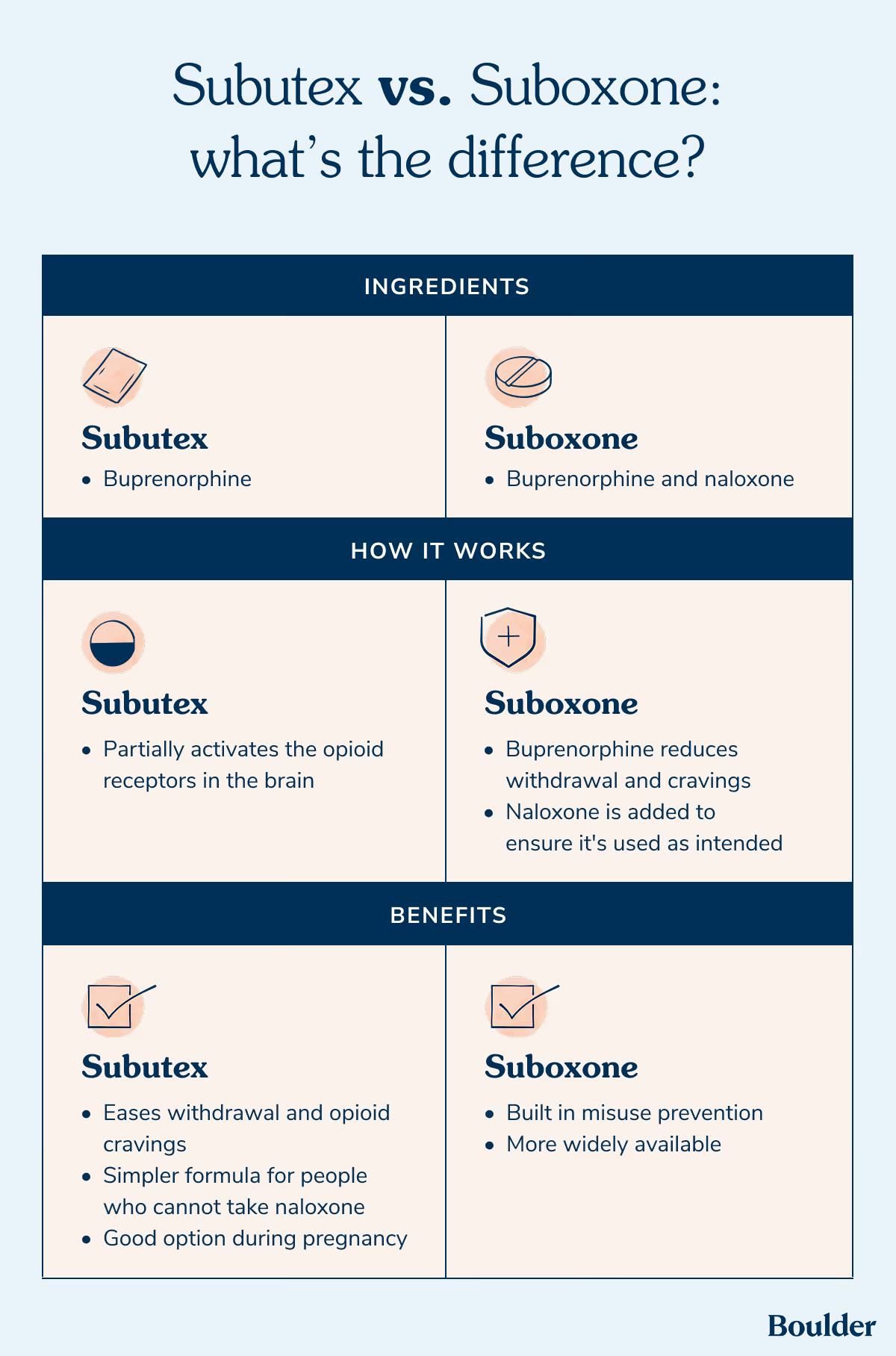
The two most common buprenorphine medications are Subutex and Suboxone. Buprenorphine is an FDA-approved, first-line treatment for opioid use disorder. While Subutex was a brand-name version that contained only buprenorphine and has since been discontinued, Suboxone adds naloxone and is now more commonly prescribed. Understanding how these medications differ and when they are typically prescribed can help you feel more confident about which option might be right for you.
According to addiction medicine physician Dr. Ayesha Appa, individual experiences can also play a role in that decision. “Like with many medications, some people simply do better on one formulation than another, and we want to honor that and work with what's most effective for each person,” she says.
In this article, we'll explore how Subutex and Suboxone work, how they differ, and what to consider when weighing each option in your own treatment.
Subutex and Suboxone are both medications that can help people who want to stop using opioids. They work in very similar ways, with both reducing cravings and withdrawal symptoms. This can make it easier for people to stop using opioids like prescription pain medications, heroin, and fentanyl.
The main thing that Subutex and Suboxone have in common is that they are both buprenorphine medications. Buprenorphine binds strongly to opioid receptors and prevents more dangerous opioids from binding to these receptors. This offers protection from an overdose if someone continues to use other opioids.
The main difference between the two medications is that Suboxone contains an added ingredient called naloxone, while Subutex, or generic buprenorphine, does not. Naloxone blocks the effects of opioids, but it’s important to call out that naloxone only activates when Suboxone isn’t taken as intended. It can also reverse an opioid overdose.
Subutex originally contained only buprenorphine. The brand name Subutex was discontinued in 2011, but generic buprenorphine (without naloxone) is still sometimes prescribed.
Given the similarities, you might wonder, is Subutex the same as Suboxone? Do they have the same effects? While Subutex and Suboxone are similar, they have important differences.
Subutex contains one active ingredient: buprenorphine. This medication works by partially activating the opioid receptors in the brain. By doing this, it is able to reduce withdrawal symptoms and cravings without the rush and sedation that full opioids cause.
The brand-name version of Subutex is no longer FDA-approved because it was discontinued in 2011. However, providers still prescribed generic buprenorphine for people who are pregnant or who can’t take naloxone for medical reasons.
The benefits of Subutex include:
Suboxone is FDA-approved and considered the standard treatment for people who want to stop using opioids. Suboxone contains two medications: buprenorphine and naloxone. Buprenorphine is what does the main work by reducing withdrawal and cravings.
“Naloxone was added to Suboxone as a deterrent to misuse, particularly injection. The idea is that if someone injects the medication rather than taking it under the tongue as prescribed, the naloxone would block the effects of buprenorphine,” explains addiction medicine physician Dr. Ayesha Appa.
When Suboxone is taken as prescribed, the naloxone doesn’t have any effect. “When taken as directed sublingually (under the tongue), the naloxone is barely absorbed and doesn't interfere with treatment,” Dr. Appa explains. But if someone tries to inject it, naloxone will block opioids’ effects and cause uncomfortable withdrawal symptoms.
The benefits of Suboxone include:
Subutex, or generic buprenorphine, is not as commonly prescribed as it used to be due to updated research that suggests Suboxone is just as safe to use during pregnancy.
Certain medical conditions may also impact which medication your provider recommends. Those with liver disease may be more sensitive to the small amount of naloxone that is absorbed under the tongue.
“It's also worth noting that buprenorphine prescribing varies across different regions of the country due to state laws and regulatory oversight, which can affect how people access these medications,” she explains.
If you are pregnant and looking to reduce your opioid use, the most important thing to know is that getting help is the best choice for you and your baby. Understanding the differences between Subutex vs. Suboxone in pregnancy can help you work with your provider to decide which option is right for you.
"Decisions about which formulation to use in pregnancy should be a shared decision between the patient and their provider, based on patient experiences, preferences, and access," Dr. Hull says.
For many years, doctors usually only prescribed Subutex during pregnancy. It wasn't clear if naloxone was safe for a developing baby or if it might cause a developing baby to experience withdrawal.
"Historically, there was a concern that the naloxone component in Suboxone could be dangerous to the developing fetus, but evidence has demonstrated that both medications can be safely used in pregnancy," Dr. Hull explains.
The good news is that research has found that babies born to people who took Suboxone during pregnancy are:
Because of this, medications for opioid use disorder (MOUD) are now recommended by major groups such as the American College of Obstetricians and Gynecologists (ACOG) and American Society of Addiction Medicine (ASAM). Dr. Hull notes that treatment with Subutex and Suboxone has similar maternal and fetal outcomes. "Some more recent evidence points to some possible benefits of combined buprenorphine-naloxone over buprenorphine only especially in terms of rates of severe neonatal opioid withdrawal syndrome," she says.
So if you are already doing well on Suboxone and find out you are pregnant, many providers now recommend staying on your medications instead of switching.
When it comes to other risks, like cesarean delivery, low birth weight, and preterm delivery, research suggests there’s no significant difference between Subutex and Suboxone. Both medications are considered safe and effective during pregnancy.
One potential risk to be aware of is neonatal withdrawal, which requires medical monitoring. “Any formulation of buprenorphine can lead to dependence in a newborn, and all newborns exposed to buprenorphine should be monitored for neonatal withdrawal symptoms,” Dr. Hull says.
This is a common question but there isn’t a one-size-fits-all answer. Neither medication is "better" than the other for everyone. “Treatment should not differ significantly between buprenorphine and buprenorphine-naloxone in terms of effectiveness, dose prescribed, or method of initiation,” Dr. Hull says.
The answer to which one is better for you depends on your body and your history. Even though Suboxone is the most common choice today, there are some reasons why your provider might opt for Subutex instead:
If you are wondering which path and dosage is right for you, the important thing is to work with your doctor.

While both medicines are safe when used as directed, they can still be used in unsafe ways. This is where the big difference between the two medications comes in:
Most people start to feel a lot better once they start on Subutex or Suboxone, but like any medication, you may have some side effects.
Dr. Appa notes that overall, there aren't any meaningful differences in terms of side effects between the two medications. "The active ingredient we're focused on in either case is buprenorphine—that's what's doing the therapeutic work," she says.
It’s also important to remember that people don’t always experience these medications in the same way. "Some people tolerate one medication better than the other due to taste or how quickly it dissolves, and some people have fewer side effects from one type of medication over another," Dr. Hull says.
Side effects are often more common when you first start taking your medication because it takes a little time for your body to get used to it. Fortunately, these side effects are usually mild and lessen as you continue taking your medication.
The most common side effects with these medications are:
In many cases, there are things you can do to help relieve these symptoms. Drink plenty of water and rest to alleviate headaches, eat a healthy diet and stay active, and talk to your doctor about the best time to take your medication so it doesn't disturb your sleep. Your doctor may also suggest some over-the-counter medications to deal with some side effects.
"If people have side effects, especially nausea or headache with administration of buprenorphine-naloxone, these symptoms may improve if they spit out their saliva after the medication dissolves to minimize absorption of naloxone in the stomach," Dr. Hull suggests.
Subutex and Suboxone can help improve your daily life and functioning shortly after starting them, but it's important to remember that recovery takes time. Knowing what to expect can help you feel more in control.
Treatment and recovery are a lot like building a house. You need to start with a strong foundation before you can build the walls and roof. The stages of recovery follow a pattern:
If you start your medication too soon, you might experience something known as precipitated withdrawal. Buprenorphine is very "sticky." It wants to grab onto any spots in the brain where opioids might latch on.
If those opioids get booted off the receptors too fast, it puts your body into an intense, immediate withdrawal. It can make you feel really sick, much like having a very bad flu. You might experience:
To minimize the risk of precipitated withdrawal, you'll wait until you're already starting to feel symptoms of withdrawal before you take your first dose of Subutex or Suboxone. That helps ensure that the opioid receptors are already empty. Comfort medications can also be prescribed to minimize the discomfort associated with withdrawal.
"This is easiest to do with a short-acting opioid like oxycodone and much harder to do for a full-agonist opioid, which can stay in the system for much longer," Dr. Hull says. Full-agonist opioids like fentanyl can stay in the system much longer, making it a challenge to start Suboxone too soon. Another option is to start buprenorphine in low doses while waiting for other opioids to clear the body.
Boulder also offers a QuickStart method that allows people to transition from full opioids to buprenorphine much faster. This method involves self-administering intranasal naloxone to clear your opioid receptors of full-agonist opioids, and then quickly taking a high dose of buprenorphine to fill the open receptors.
QuickStart is the quickest known way to start buprenorphine, with patients often reaching their stable dose within hours. It also causes relatively intense, but short and managed withdrawal—so it all depends on your goals and what resources you have on hand.
Whichever medication you choose or how you start, buprenorphine can help your brain start to heal and recover from opioid use. Taking them long-term makes the cravings go down, so you're not thinking about drugs all the time.
While it can be helpful to hear about other people's experiences with medications, sometimes what you hear includes things that might be a bit misleading. Let's clear up some of the most common myths about Subutex and Suboxone.
People sometimes think that since Subutex doesn't have naloxone in it, it's stronger or works better. This isn't true because both medications contain the exact same amount of the active ingredient, buprenorphine. If you take an 8mg tablet of Subutex and an 8mg film of Suboxone, your brain is getting the same amount of medication. Suboxone isn't stronger; it just contains an extra safety feature that doesn't affect how the active ingredient works in the body.
Even so, starting buprenorphine can be challenging for people who are currently using fentanyl, Dr. Appa says. "Buprenorphine is a partial opioid agonist with high affinity for opioid receptors, and the transition from a full agonist like fentanyl can be uncomfortable for some patients," she explains.
While some people mistakenly attribute those effects to naloxone, they're usually due to buprenorphine itself. “That said, when patients tell us they've had trouble with one formulation versus another, we take that seriously and work with them to find what works best,” says Dr. Appa.
Since naloxone blocks the effects of Suboxone if it is injected, people sometimes mistakenly think that it's also what's keeping them from having cravings. In reality, your body doesn't do much with naloxone when it's taken under the tongue. It only becomes active if it's used by injecting it. It's the buprenorphine that is actually stopping the cravings so that you can feel steadier and less distracted by thinking about opioids.
Since Subutex and Suboxone are partial opioids, some people confuse taking them with just using another type of drug. But this just isn't true. These medications don't cause the rush and sedation that opioids do.
They also don't lead to the loss of control that people experience from an addiction. They help you stay stable, clear-headed, and focused on recovery. Taking medication to treat addiction is like taking medication for other chronic illnesses, like asthma or diabetes.
"Something that comes up a lot with patients is fear and stigma around taking medications that treat opioid addiction, like Suboxone. I get that," says Crystal, a peer support specialist who has taken Suboxone as part of her own recovery journey. "So when I talk to patients who are on the fence and aren’t sure what they want to do, I listen and make sure they’re being heard. Because what they’re feeling is real. I’ve felt that too."
People sometimes think that taking a medication with more ingredients might lead to more side effects. However, when taken as prescribed, both Suboxone and Subutex are equally safe because buprenorphine is the only active ingredient.
In some cases, Suboxone is considered the safer option because it’s less likely to be used in ways it wasn't prescribed. That's why Subutex is usually only prescribed for specific reasons, such as if a person has an allergy to naloxone.

Starting treatment is a big step toward a healthier life. The first step is talking to your provider and deciding which medication is right for you. At Boulder, getting started is as simple as downloading the app. You'll connect with same-day virtual care that happens completely on your phone. Here's a quick start guide to explain what that process looks like:
How you start your medication will also be tailored to your needs and involve shared decision-making between you and your clinician. Many follow a standard induction schedule that involves waiting for early withdrawal symptoms before starting buprenorphine medication.
Some people may opt for Boulder's QuickStart approach, which can make transitioning from opioids to Suboxone or Subutex much faster.
Your own individual experience will be tailored to your needs, including the amount of medication you'll take and how quickly you'll start. Those are all things you can talk about with a Boulder clinician.
Fortunately, most insurance plans cover addiction treatment, including Medicaid and Medicare. Since Suboxone is a first-line treatment, it is usually easy to get covered by insurance, but you can also use our tool to see if Boulder takes your insurance.
What if you don't have insurance? Boulder offers several self-pay options that can help you afford your medication.
Since Subutex was discontinued as a brand-name product but is available as a generic buprenorphine, it is generally affordable. However, insurance companies may sometimes require a prior authorization note from your doctor to explain why you are taking Subutex instead of Suboxone.
Some states may also have regulations that make Subutex harder to access. Some may require prior authorization, have dosing limits, or even prohibit prescribing buprenorphine-only medication except in very specific situations. For example, Boulder Care cannot prescribe Subutex in states like Ohio, North Carolina, and New Mexico due to the limited availability of Subutex in many pharmacies.
Both Subutex and Suboxone are "sublingual" medications, which means they dissolve under your tongue. They should not be swallowed like some other pills or capsules.
Your provider will also give you information on how to take your medication. For it to work best, they suggest not eating, drinking, or smoking for around 15 to 30 minutes after it dissolves. Be sure not to swallow it whole, since this can affect how it enters your body.
Following your provider's instructions is important. Sticking to your schedule for taking doses, and taking the proper dosage, will make sure that the medication is working the way it is supposed to.
Choosing between Subutex and Suboxone can feel like a big decision, but the key is to work with your provider to find the treatment that is right for you.
Both medications work well and are excellent tools to help you stop feeling cravings and withdrawal symptoms. Both are safe, even during pregnancy.
At Boulder, we believe that medication can help you reach your recovery goals. Our team is here to listen without judgment and create a plan that works for you and your life. We know that the recovery journey can look different for everyone. "There are multiple pathways to recovery," explains Danielle, a peer supervisor at Boulder. "I let people know: what works for me doesn't necessarily work for the next person...What's important is to do what's best for you."
Ready to start? Whether you have questions about which medication to take or are ready to start your first appointment today, we're ready to help through the Boulder app. You can also call 888-422-6530 to speak with a care team member and learn more.
Suboxone is generally considered the safer choice because it contains naloxone, which lowers the risk for misuse. Any medication can be misused if it isn't taken as directed, but evidence has shown that buprenorphine is a safe and effective treatment for opioid use. Both Subutex and Suboxone are safer than using full opioids like prescription pain pills, heroin, and fentanyl.
Subutex was discontinued as a brand-name product by the manufacturer in 2011 due to concerns over a potential higher risk for misuse. The active ingredient in Subutex, buprenorphine, is still available as a generic prescription.
Subutex is still often prescribed during pregnancy. In the past, doctors weren’t sure about how naloxone, the added ingredient in Suboxone, might affect a pregnancy or the developing baby. More recent research suggests that Suboxone is just as safe as Subutex during pregnancy.
If you are taking Subutex or another medication containing buprenorphine, you should avoid central nervous system depressants like alcohol and benzodiazepines such as Xanax and Valium. Combining these medications can slow breathing and increase the risk of an overdose.
You should also avoid other opioids, muscle relaxers, and kratom. Buprenorphine can also affect how some other medications work in the body, so always tell your prescriber about any other medications you are taking.
At Boulder Care, we’re committed to providing clear, evidence-based information about opioid and alcohol use disorder recovery. Learn more about our editorial standards and medical review process.