
From the outside, Danielle Bellosi’s suburban Philadelphia upbringing looked stable. But in reality, she lived in an unpredictable home where substance use was common. She first tried alcohol at age 12. “From a very young age,” she says, “I felt uncomfortable in my own skin.” This led to more experimentation with alcohol and marijuana.
Bellosi didn’t have the language for what was going on back then, but now she knows childhood trauma played a role in her experience with addiction. Eventually, she received a prescription for the opioid medication Vicodin after dental work as a teen.
“From there,” she says, “it became anything that I could change how I felt. If it was available and promised relief, I was open.” By age 18, she was injecting heroin.
She first learned about medication-assisted treatment (MAT) at 20. She started taking methadone. This treatment plan worked for her for a while. But she says, “the stigma was overwhelming.” Ultimately, she tapered off the medication.
“Heroin returned, and benzodiazepines entered the picture,” she says. “Things unraveled quickly.” She lost her car and her job as a medical assistant and phlebotomist.
Eventually, she was prescribed Suboxone, which contains buprenorphine. “Buprenorphine saved my life—period,” she says.
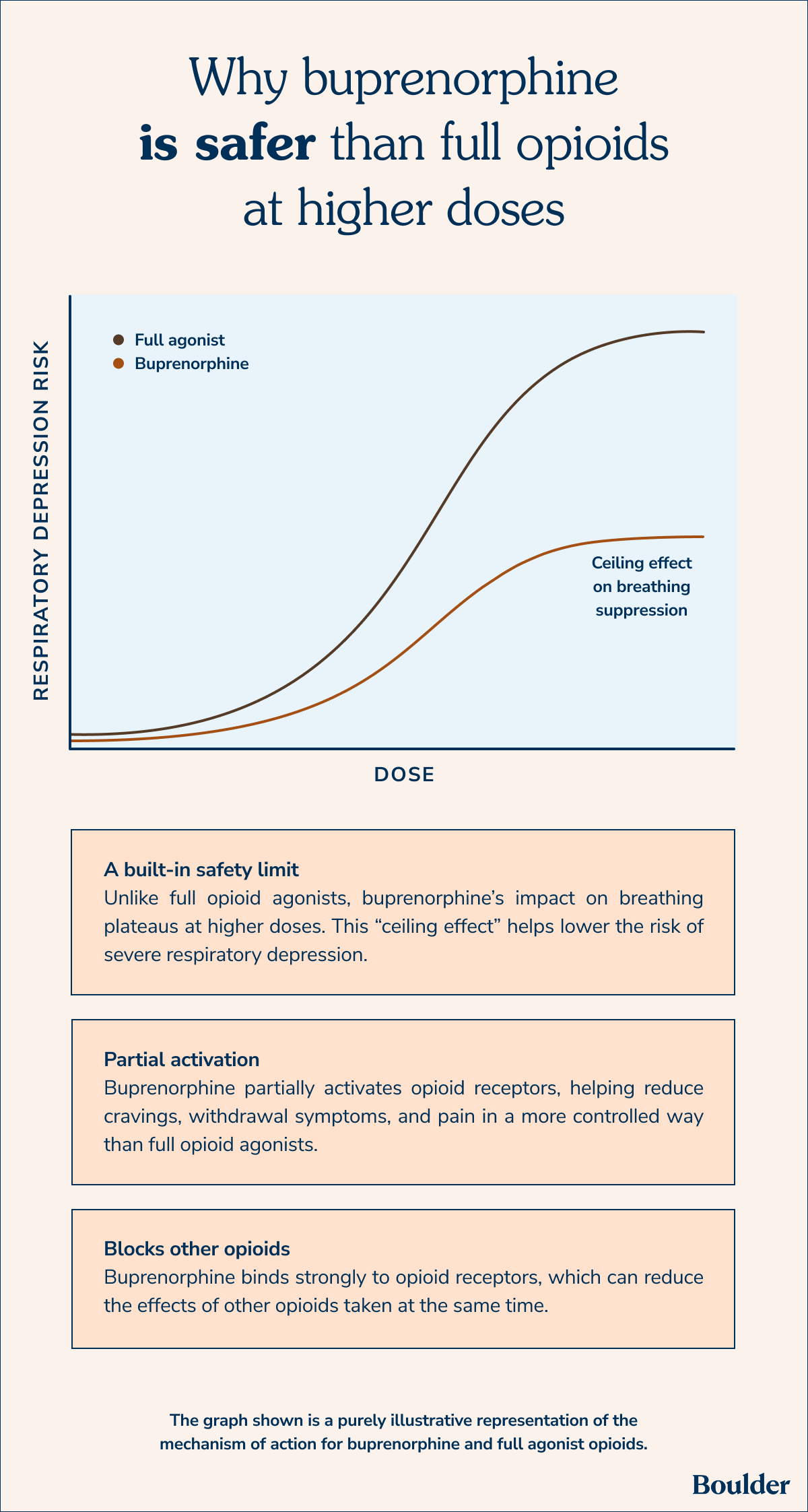
Buprenorphine is a medication used to treat opioid use disorder and chronic pain. It is an opioid itself. But it helps reduce cravings and withdrawal symptoms. And it blocks the effects of other opioids. For these reasons, it can be a lifesaving medication while aiding recovery.
Bellosi adds, “Buprenorphine gave me stability when my body and brain couldn’t regulate on their own yet. It reduced the constant fear of withdrawal and cravings, allowing me to focus on healing instead of just surviving.”
In this article, we explore what buprenorphine is, buprenorphine for opioid use disorder (OUD), buprenorphine side effects, and more.
Buprenorphine is an FDA-approved prescription medication used to treat opioid use disorder (MOUD). It’s also prescribed to treat chronic pain.
Is buprenorphine an opioid? The answer is yes. But buprenorphine helps reduce cravings and withdrawal symptoms after you stop taking other opioids. It also blocks the effects of other opioids. For these reasons, buprenorphine can be a lifesaving medication while aiding recovery and improving your quality of life.
“I was taught to believe that if I was taking medication, I wasn’t truly in recovery,” Bellosi says. “I wasn’t welcomed into traditional recovery spaces that viewed complete abstinence as the only valid path.”
She adds, “What I didn’t realize at the time, and couldn’t fully appreciate until years into my recovery, was the profoundly positive role buprenorphine played in my life. It kept me alive.”
Buprenorphine is a partial opioid agonist. An agonist is a substance that activates receptors in the body. The receptors in the body and brain that buprenorphine activates are called mu-opioid receptors (MOR). These receptors affect pain, comfort, and mood. Buprenorphine partially activates these receptors—just enough to reduce withdrawal and cravings. Because buprenorphine only partially activates MOR, it does not create a “high” like other opioids.
Stephen A. Martin, EdM, FAAFP, FASAM, is an associate professor of family medicine and community health at the University of Massachusetts Medical School. He’s also the senior advisor for research and practice at Boulder Care.
He says, “We have over half a century of understanding about buprenorphine that is helpful, both from patients and in physiologic studies.”
He adds, “Buprenorphine is able to take up space in the cell receptor (like one of many doorbells for the cell). And it attaches very strongly to this receptor, making it hard for other opioids (like fentanyl or heroin) to attach themselves. So buprenorphine, given a chance, attaches to cells instead of fentanyl or heroin and then has a calmer effect.”
Dr. Martin says that everyone has a unique set of reasons for taking buprenorphine. Exploring potential reasons can help you better understand how buprenorphine works.
Replacement
One way is to think of it as replacing something your body needs. A good example is diabetes, where a person's body doesn't produce enough insulin. You take insulin as medication to keep your blood sugar levels stable and stay healthy. Opioid addiction means your body needs opioids to avoid becoming sick. Buprenorphine steps in to replace stronger opioids, such as heroin or fentanyl. Think of buprenorphine as a medication to treat a disease.
A safer substitution
“This is intentional opioid replacement.” Dr. Martin explains. Buprenorphine is an opioid to treat opioid use disorder. But, as one of the veteran psychologists I work with points out, it’s replacing an opioid that hurts you—or even kills you—with one that doesn’t.”
Improved well-being and quality of life
“‘I feel normal again!’” is a phrase of gratitude I hear again and again. When there’s a good match with a dose, people shouldn’t have cravings or withdrawals. They can shape their lives and start feeling better. It can’t solve everything, for sure. But patients say it makes things so much easier.”
The U.S. Food and Drug Administration (FDA) has approved buprenorphine for two reasons:
If you’re beginning treatment for OUD with buprenorphine, then you will likely start taking it about 12 to 24 hours after your last use of other opioids. This buffer timeframe is important. Taking buprenorphine too early in the process can cause precipitated withdrawal (intense withdrawal).
Depending on your unique recovery situation, your dose may change after you’ve been stabilized on the medication.
Buprenorphine treatment comes in several different forms:
Buprenorphine medication is also available under several different brand names that vary by indication or purpose. These various medications are explained below:
Medications indicated for OUD + Pain: buprenorphine and naloxone
Medications indicated for OUD: buprenorphine
Medications indicated for pain: buprenorphine
*Boulder Care offers multiple formulations (marked with an asterisk above), both brand-name and generic. It depends on the patient's insurance and preference.
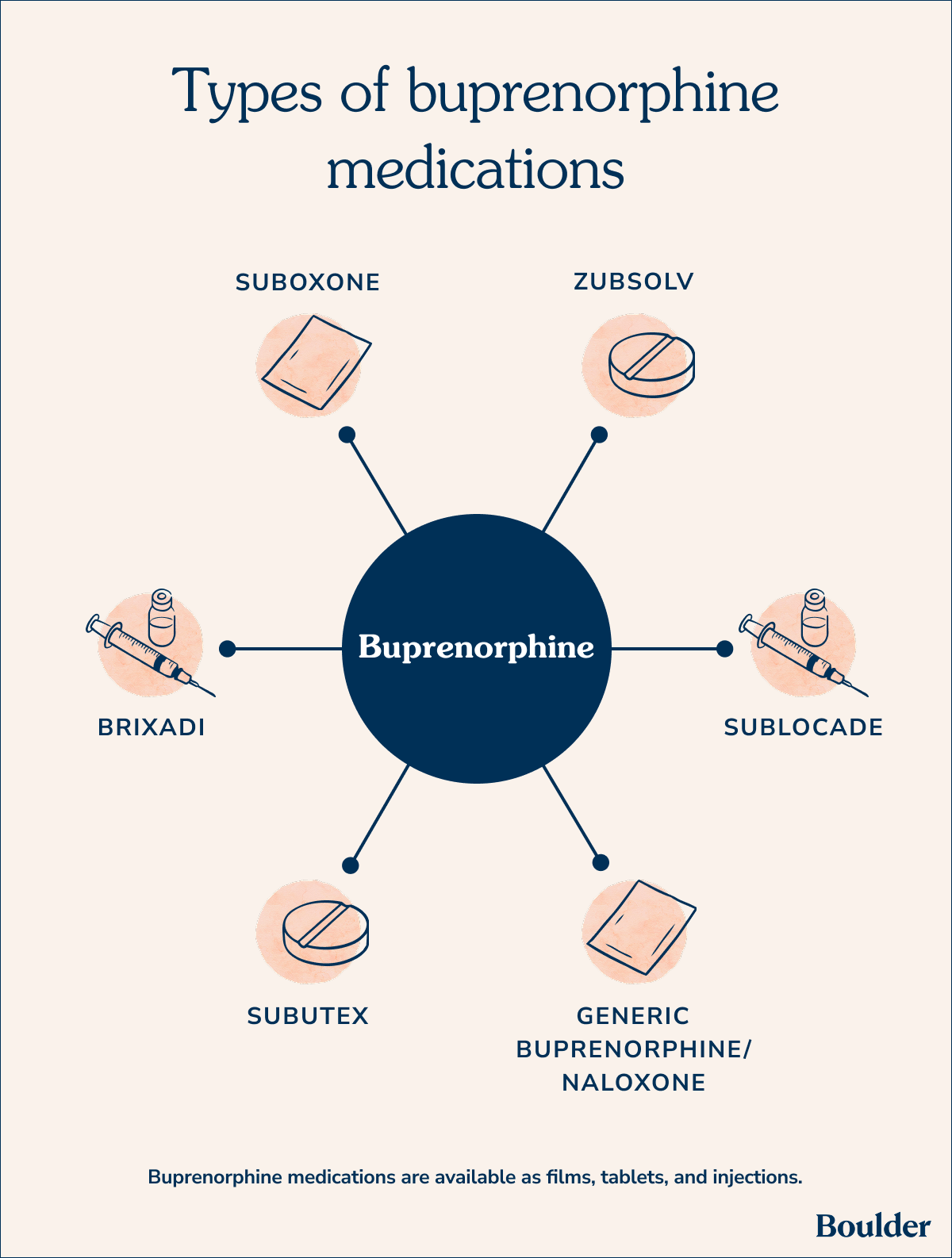
Note that you aren’t seeing methadone on the list above. Methadone is a full opioid agonist, whereas buprenorphine is a partial opioid agonist.
You’re not alone if all the medication names and terms feel a bit confusing. Buprenorphine is a medication sold under the brand name Suboxone. Suboxone also contains naloxone. Naloxone is a built-in safety feature to help ensure that Suboxone is used as intended.
As with any medication, buprenorphine has some potential side effects. Not everyone who takes this medication will experience side effects. If you do experience side effects, talk to the provider who prescribed you the medication.
Boulder Care has a resource page for managing minor side effects. You might find a solution that works for your unique situation. For example, a special toothpaste can help you manage dry mouth.

So, what does taking buprenorphine feel like? “Buprenorphine felt like a safety net,” Bellosi says. I understood how it worked in my brain, and I could feel its grip on cravings—and the fear of withdrawal—begin to loosen, even during periods when my recovery path wasn’t linear. It calmed both my mind and my body, giving me the ability to function when I would otherwise have been sick and debilitated.”
So how does the process work? Buprenorphine treatment is not one-size-fits-all. Boulder Care offers a protocol for taking buprenorphine. It involves confirming you are in withdrawal before taking your first dose, then following additional steps.
“Many patients choose the transition method we’ve used the past 20 years,” Dr. Martin says. “Others take more buprenorphine faster (over the course of a few hours) and that works better for them.”
These approaches may not be the right option for you. “I wish we could predict the best method for everyone and that there were approaches with no risk, but this isn’t the case,” he says. Sometimes side effects occur.
“We can for sure say that just about everyone can find a way onto buprenorphine,” he adds, “and that a trusted guide—in our case, often a Peer Recovery Specialist—makes this more possible.”
Bellosi is now a Peer Supervisor at Boulder Care. She says, “Truly honoring recovery means respecting what that process looks like for each person and creating spaces where people can be exactly where they are—without pressure or judgment, without added shame or guilt, and without punishment or consequences—as they decide where they want to go.”
How long you take buprenorphine depends on factors unique to you and your situation. Research indicates that taking buprenorphine for less than 90 days for OUD is not as effective as taking the medication long term.
Again, duration is not one-size-fits all. It’s about what’s right for you in the moment. You might decide to only take it temporarily.
If you're curious about whether Suboxone could be a good fit, Boulder is here to help. Call 888-422-6530 to speak with a care team member and learn more about getting started.
Buprenorphine is a medication that can help meet you where you are with opioid use disorder.
“I’ve prescribed hundreds of different medications over my career and there are only a handful that have the dramatic improvement buprenorphine (and its alternative, methadone) allows,” Dr. Martin says. “People not only feel better, they feel [like] themselves again—not just for a day, but for weeks, months, years, and the rest of their life.”
In addition, buprenorphine is part of harm reduction regarding OUD. “At the right doses and if it's active in the body, buprenorphine also offers some protection against harms of fentanyl, like overdose, if a person returns to use.”
Bellosi agrees. “It took working in the recovery industry to truly understand that there are multiple pathways to recovery and that no single approach holds all the answers,” she says. What I know now is simple and unwavering: As long as there is a pulse, there is hope.”
If you're curious about whether Suboxone could be a good fit, Boulder is here to help. Call 888-422-6530 to speak with a care team member and learn more about getting started.
Yes, buprenorphine is an opioid medication used to treat opioid use disorder. But buprenorphine only partially activates opioid receptors, leading to milder effects. It also helps reduce cravings and withdrawal symptoms. And it blocks the effects of other opioids.
Overdose on buprenorphine is possible. However, it is rare. When it occurs, it is usually because of exposure to other substances at the same time that can cause respiratory depression.
Yes, buprenorphine is generally covered by private insurance, Medicaid, and Medicare. But coverage depends on your specific insurance plan.
At Boulder Care, we’re committed to providing clear, evidence-based information about opioid and alcohol use disorder recovery. Learn more about our editorial standards and medical review process.